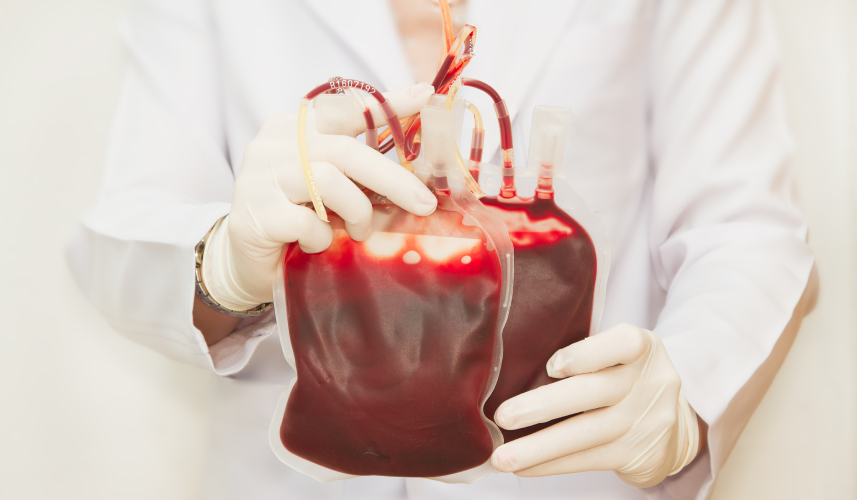
Much of the focus for making cell and gene therapies (CGTs) accessible and commercially viable has looked downstream at manufacturing, logistics, geography, centralization, and even intellectual property. However, the vast majority of ex vivo advanced therapies share the same starting point — blood — and the future of CGT rests on our ability to improve how we get what we need from patients’ and donors’ blood.
Cellular starting material that will be used to produce blood cell-based therapies is isolated through automated apheresis, but that’s not really the start of the process. For autologous therapies, like gene-edited therapies for sickle cell disease made from hematopoietic stem cells (HSCs), patients may undergo multiple rounds of therapeutic apheresis and leukodepletion months before receiving the actual therapy. While these sessions often take place at the medical center where a patient is receiving treatment, there’s growing opportunities for apheresis to happen closer to home — at blood centers, for example, where therapeutic or donor apheresis is already performed.
The starting point for allogeneic therapies is the donor recruitment process. Blood centers are given specific criteria to meet depending on the drugmaker’s requirements. These can relate to some combination of donor characteristics including general health, past exposure to specific viruses, or ability to produce the desired cells. Recallability is also crucial to ensure a steady supply of starting material for clinical testing or commercial consistency.
Blood for CGT
In the CGT space, blood is a tool, a therapy, and a gift. For therapeutics, automated apheresis is used to isolate blood components like lymphocytes and HSCs that will become the starting material that is to be transformed into an ex vivo therapy.
Outside of autologous therapies, most of the blood used comes from healthy donors — whether for enabling device development, safety testing, manufacturing process runs, or as the starting point for allogeneic therapies themselves.
Donor material sourcing resembles traditional practices in the blood banking industry. Blood centers maintain and manage recallable donor lists — and increasingly, these include individuals who provide starting material for advanced therapies. Like traditional blood donors, these individuals contribute biological material through apheresis or other procedures, and are selected based on defined eligibility criteria.
“The same operational models used to support whole blood and platelet donation, such as donor recall systems, scheduling infrastructure, and follow-up protocols, are now being adapted to support consistent sourcing of starting material for CGTs,” says Jeff Wren, vice president of biotherapies at the Association for the Advancement of Blood & Biotherapies (AABB). “While the donation requirements are often more specific, the underlying systems are familiar to blood centers.”
As a result, many of the challenges faced by the blood industry writ large are shared for CGT applications. The biggest is the issue of supply. Blood banks in the U.S. are seeing an aging donor base and changing behavior among demographics.
“In the last ten years, we have seen a 36% decline in donors under the age of 30. At the same time, in 2024, 24% of donors giving at a BCA center were 60 or older,” says Bill Block, president and CEO of Blood Centers of America (BCA). This changing landscape has made it harder to recruit new donors, and harder to get them to come back regularly.
While CGT sourcing challenges are similar in broad strokes, the field often demands more specific components with stringent restrictions — leading to a reliance on ‘super donors’ who consistently donate in both quality and quantity.
CGT-specific challenges
There are some issues in CGT that are unique to these donors and to how quality is maintained. One main challenge is obtaining large pools of medically cleared, fit and willing donors, who are committed to consistent donation because they understand the long-term benefits of donating cells for research and development.
There is a lot of consideration for patient safety during the complex processes involved with CGTs. But as allogeneic therapies progress through the clinic and increasingly commercialize, donor safety must receive the same kind of emphasis.
Although apheresis is so safe that it is commonly performed in blood centers, there is one practice that carries additional long-term risks: stem cell mobilization. Mobilization for therapeutics development is fairly common and acceptable if done under an Institutional Review Board (IRB)-approved study. Unfortunately, some organizations overuse it without fully informing donors. Stricter rules may be needed.
It is crucial that donors know what they are getting into. Due to the still-evolving technical, ethical, and regulatory landscape in CGT, there is a lack of standardization for informed consent. Ensuring consent is done appropriately, with care and rigor, is paramount for any donation. That means forms should be clear, and no one should be consented under duress like during labor or while in a rush — especially non-native speakers.
Finally, donation should never affect medical care. For example, with umbilical cord blood, the practice of delaying cord clamping has shown to be beneficial to newborns but results in smaller blood volumes collected. To ensure ethical practices are in place, it is incumbent on organizations to enforce medical guidelines that prioritize donor health, and developers need to audit their suppliers’ entire donation process.
The other category for special consideration with CGTs is cell quality, which can impact how difficult it is to manufacture a product that meets the target dose and appropriate function of the product.
“Living cells are complex units that have diverse genetics, gene expression, and phenotype/functional differences that all affect how long the cell will live and how it will behave in the target environment,” says Mindy Miller, Ph.D., head of scientific development and engagement, global therapy innovations at Terumo Blood and Cell Technologies.
Unlike whole blood donations, where the clear end goal is about a pint of blood, CGT requirements for a leukopak are more complex and can be difficult to achieve. A drugmaker may require a specific minimum number of cells from apheresis, a particular challenge if rare cell types are needed such as T-regulatory cells. Sometimes, HLA matching may be needed for particular treatments or starter material, meaning access to a large register of potential donors is crucial. There can also be less understood donor differences that impact the end cell product.
In many cases, therapies require starting material that isn’t frozen and must begin manufacturing within a day. This creates tight logistical constraints, as cells must be processed quickly to preserve function and quality. Extended transit times or handling delays can lead to cellular degradation and reduced viability, increasing the risk of manufacturing failure.
“This is particularly relevant for autologous therapies, where patients, often with advanced disease, may only be able to donate once,” says Wren. “Any loss of viability due to shipment delays or handling issues can jeopardize the entire treatment.”
Traditional inspiration
Despite distinctions, much of what the industry has learned from traditional blood banking is useful as demand within the CGT field continues to expand.
“Blood centers have long been competing for people’s time in an effort to secure sufficient voluntary blood donations,” says Becky Butler Cap, senior vice president, Vitalant. “We think that experience informs some ways forward in CGT.”
When it comes to challenges securing donors, the first solution is education.
“Most people don’t know that there are multiple lifesaving components in blood, and that these components have a vast array of uses — from helping trauma victims to pregnant moms to cancer patients,” says Betzy Gonzalez, director, scientific and technical operations, America’s Blood Centers (ABC). “Today, most people are unaware of how cell therapies can save lives, let alone how they are made. Understanding what happens after your blood donation can be an excellent motivator for repeat donations. Highlighting the profound impacts that blood donations have on patients’ lives is a key driver of donors, given the historically altruistic nature of the donor base.”
However, there are some distinctions that should not be ignored. For one, the apheresis process requires a much larger commitment of time than whole-blood donation: blood is removed, components are isolated, and unneeded components are reinfused. Also, a one-time cell-based therapy today may be priced from hundreds of thousands to millions of dollars — a commercial product valued a magnitude higher than a pint of blood. A donor whose gift becomes a drug might feel entitled to some compensation. At the same time, no one in the field wants to commodify human beings.
In some regions, small incentives like gift cards, movie tickets, or free meals may be considered acceptable, and can encourage repeat apheresis donations. Compensating these donors appropriately, especially for rarer blood types or specific components like immune cells, could significantly increase the donor pool, ensuring a stable and diverse blood supply. Today, however, the evolving international ethical and regulatory landscapes are a patchwork of competing ideas.
“Both cell therapy developers and donors prioritize and value consistency and reliability. Advance scheduling helps donors plan effectively, allowing them to arrange work commitments, childcare, and other responsibilities around their donation appointments,” says Gonzalez. “This approach not only increases donor show rates but also fosters a sense of commitment, significantly enhancing the likelihood of repeat donations and long-term engagement with their blood center.”
Recognizing donors’ contributions and valuing their time creates a positive experience, encouraging continued participation and ultimately benefiting the CGT industry.
“When managing donors, it’s important to remember that they are human beings, not quotas. A personal connection with donors goes a long way in forming and maintaining a long and mutually beneficial relationship,” says Gonzalez.
Inventive solutions
Donation should be convenient, easy and rewarding, which will yield better donor satisfaction levels. Technology plays a role here, ideally enabling a seamless digital experience for donors to be invited to give blood and components, make an appointment, and receive confirmation of the difference made by their potentially life-saving contributions.
That’s just the tip of the tech iceberg. One effort that may help entice younger donors employs virtual reality. BCA sponsored mixed-reality technology in an innovative program that allows blood donors to visit a digital world while remaining fully aware of their surroundings for a safe, relaxing donation. “A recent study showed that the mixed-reality headsets helped reduce donor anxiety and enticed them to give blood repeatedly,” says Block. Communication channels like social media can also improve outreach.
Blood centers now utilize automated platforms to efficiently collect, test, and distribute blood products for transfusion.
“Innovative hardware, connectivity software, and analytic tools help blood centers manage and optimize their operations,” says Chetan Makam, general manager, global blood solutions, Terumo BCT. “These automated systems collect or prepare blood for transfusion, ensuring blood products meet regulatory requirements. Data from user experiences can further be analyzed using algorithms that can help optimize and specialize processes.”
In one example, an expert at Harvard Medical School was able to leverage such learnings to improve the apheresis process for patients with sickle cell disease, whose blood can sometimes be challenging to process. This type of optimization is critical for isolating the type of HSCs used today in commercial autologous cell-based therapies, collecting more cells quickly and allowing patients to spend less time undergoing apheresis.
The donor experience is only one area where tech can change the landscape. Another is the quality and usability of the blood product. “Blood expires, and external conditions can impact how the quality of components degrade over time. Meeting demand requires a constant, predefined influx of donors,” says Makam.
For this reason, more commercial and late-stage clinical therapies use frozen cellular materials — leukopaks, cord blood, or isolated cells — to preserve cell viability and quality, simplify logistics, and allow for more flexible manufacturing timelines. Technology is improving the way the materials are frozen and thawed, and new research is helping identify the best practices for consistent quality.
“Where fresh materials are unavoidable, minimizing transport time and handoffs and using validated shipping methods with tight controls on temperature and shipper orientation can mitigate risks and maintain cellular integrity,” says Wren. Logistics software, potentially supported by AI, can help optimize the shipping process.
What lies behind these many blood solutions, and those still to surface, is collaboration. The industry must work together to ensure the astonishing discoveries of lifechanging therapeutic technologies can reach its maximum potential through widespread patient access.
Subscribe to our e-Newsletters
Stay up to date with news, articles and insights relevant to cell and gene therapy development and manufacturing. Plus, get special offers from Cell & Gene Therapy Review delivered right to your inbox!
Sign up now!